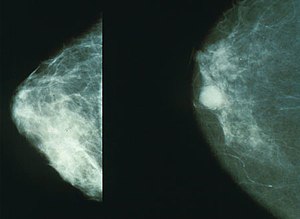
Breast cancer
| Breast cancer | |
|---|---|
| ICD-10 | ICD10 F84.0-F84.1 |
| ICD-9 | 174
-175 |
| OMIM | 114480 |
| MedlinePlus | 000913 |
Breast cancer is a cancer of the glandular breast tissue.
Worldwide, breast cancer is the fifth most common cause of cancer death (after lung cancer, stomach cancer, liver cancer, and colon cancer). In 2005, breast cancer caused 502,000 deaths (7% of cancer deaths; almost 1% of all deaths) worldwide.[1] Among women worldwide, breast cancer is the most common cancer.[1]
In the United States, breast cancer is the most prevalent cancer in women, and the second most common cause of cancer death in women (after lung cancer). In 2007, breast cancer is expected to cause 40,910 deaths (7% of cancer deaths; almost 2% of all deaths) in the U.S.[2][3] Women in the U.S. have 1 in 8 lifetime chance of developing invasive breast cancer and a 1 in 33 chance of breast cancer causing their death.[3]
The number of cases has significantly increased since the 1970s, a phenomenon partly blamed on modern lifestyles in the Western world.[4][5] Because the breast is composed of identical tissues in males and females, breast cancer also occurs in males, though it is less common.[6]
History
Breast cancer may be one of the oldest known forms of cancer tumors in humans. The oldest description of cancer (although the term cancer was not used) was discovered in Egypt and dates back to approximately 1600 BC. The Edwin Smith Papyrus describes 8 cases of tumors or ulcers of the breast that were treated by cauterization, with a tool called "the fire drill." The writing says about the disease, "There is no treatment."[8] For centuries, physicians described similar cases in their practises, with the same sad conclusion. It wasn't until doctors achieved greater understanding of the circulatory system in the 17th century that they could establish a link between breast cancer and the lymph nodes in the armpit. The French surgeon Jean Louis Petit (1674-1750) and later the Scottish surgeon Benjamin Bell (1749-1806) were the first to remove the lymph nodes, breast tissue, and underlying chest muscle. Their successful work was carried on by William Stewart Halsted who started performing mastectomies in 1882. He became known for his Halsted radical mastectomy, a surgical procedure that remained popular up to the 1970s.
Types
These are the pathological and clinical categories of breast cancer. There can be overlap between these categories; for example, a ductal carcinoma can also be an inflammatory breast cancer.
- Ductal carcinoma 65-90%
- Lobular carcinoma 10%
- Inflammatory breast cancer
- Medullary carcinoma 5%
- Colloid carcinoma 2%
- Papillary carcinoma 1%
- Metaplastic carcinoma
Symptoms
Early breast cancer can in some cases present as breast pain (mastodynia) or a painful lump. Since the advent of breast mammography, breast cancer is most frequently discovered as an asymptomatic nodule on a mammogram, before any symptoms are present. A lump under the arm or above the collarbone that does not go away may be present. Other possible symptoms or medical signs include nipple discharge, bleeding from the nipple, new nipple inversion, and changes in the skin overlying the breast, often resembling an orange peel, known as peau d'orange Template:Fact. When breast cancer associates with skin inflammation, this is known as inflammatory breast cancer. In inflammatory breast cancer, the breast tumor itself is causing an inflammatory reaction of the skin, and this can cause pain, swelling, warmth, and redness throughout the entire breast.
Changes in the appearance or shape of the breast can raise suspicions of breast cancer.
Another reported symptom complex of breast cancer is Paget's disease of the breast. This syndrome presents as eczematoid skin changes at the nipple, and is a late manifestation of an underlying breast cancer.
Most breast symptoms do not turn out to represent underlying breast cancer. Benign breast diseases such as fibrocystic mastopathy, mastitis, functional mastodynia, and fibroadenoma of the breast are more common causes of breast symptoms. The appearance of a new breast symptom should be taken seriously by both patients and their doctors, because of the possibility of an underlying breast cancer at almost any age.
Occasionally, breast cancer presents as metastatic disease, that is, cancer that has spread beyond the original organ. Metastatic breast cancer will cause symptoms that depend on the location of metastasis. More common sites of metastasis include bone, liver, lung, and brain. Unexplained weight loss can occasionally herald an occult breast cancer, as can symptoms of fevers or chills. Bone or joint pains can sometimes be manifestations of metastatic breast cancer, as can jaundice or neurological symptoms. Pleural effusions are not uncommon with metastatic breast cancer. Obviously, these symptoms are "non-specific," meaning they can also be manifestations of many other illnesses.
Epidemiologic risk factors and etiology
Epidemiological risk factors for a disease can provide important clues as to the etiology of a disease. The first work on breast cancer epidemiology was done by Janet Lane-Claypon, who published a comparative study in 1926 of 500 breast cancer cases and 500 control patients of the same background and lifestyle for the British Ministry of Health.Template:Fact
Today, breast cancer, like other forms of cancer, is considered to be the final outcome of multiple environmental and hereditary factors.
- Lesions to DNA such as genetic mutations. Exposure to estrogen has been experimentally linked to the mutations that cause breast cancer.[9] Beyond the contribution of estrogen, research has implicated viral oncogenesis and the contribution of ionizing radiation.
- Failure of immune surveillance, which usually removes malignancies at early phases of their natural history.
- Abnormal growth factor signaling in the interaction between stromal cells and epithelial cells, for example in the angiogenesis necessary to promote new blood vessel growth near new cancers.
- Inherited defects in DNA repair genes, such as BRCA1, BRCA2 and p53.
Although many epidemiological risk factors have been identified, the cause of any individual breast cancer is often unknowable. In other words, epidemiological research informs the patterns of breast cancer incidence across certain populations, but not in a given individual. Approximately 5% of new breast cancers are attributable to hereditary syndromes, while no etiology is known for the other 95% of cases.[10]
Age
The risk of getting breast cancer increases with age. A woman who lives to age 90 has a lifetime risk of about 14.3%, or one in seven.[11] The probability of breast cancer rises with age, but breast cancer tends to be more aggressive when it occurs in younger people. One type of breast cancer that is especially aggressive and that occurs disproportionately in younger people is inflammatory breast cancer. It is initially staged as Stage IIIb or Stage IV. It also is unique because it often does not present with a lump, so it is often undetected by mammography or ultrasound. It presents with the signs and symptoms of a breast infection like mastitis, and the treatment is usually a combination of surgery, radiation, and chemotherapy.
Gender
Men have a lower risk of developing breast cancer (approximately 1.08 per 100,000 men per year), but this risk appears to be rising.[12]
Heredity
In 5% of breast cancer cases, there is a strong inherited familial risk.[13]
Two autosomal dominant genes, BRCA1 and BRCA2, account for most of the cases of familial breast cancer. Family members who harbor mutations in these genes have a 60% to 80% risk of developing breast cancer in their lifetimes.[13] Other associated malignancies include ovarian cancer and pancreatic cancer. If a mother or a sister was diagnosed breast cancer, the risk of a hereditary ‘’’BRCA1’’’ or ‘’’BRCA2’’’ gene mutation is about 2-fold higher than those women without a familial history. In addition to the BRCA genes associated with breast cancer, the presence of NBR2, near breast cancer gene 1, has been discovered, and research into its contribution to breast cancer pathogenesis is ongoing.Cite error: Invalid <ref> tag; invalid names, e.g. too many
Commercial testing for ‘’’BRCA1’’’ and ‘’’BRCA2’’’ gene mutations has been available since at least 2004. Genetic testing for BRCA gene mutations is conducted exclusively by Myriad Genetics, located in Salt Lake City.
Diet
Dietary influences have been proposed and examined, and recent research suggests that low-fat diets may significantly decrease the risk of breast cancer as well as the recurrence of breast cancer.[14] Another study showed no contribution of dietary fat intake on the incidence of breast cancer in over 300,000 women.[15] A randomized controlled study of the consequences of a low-fat diet, the Women's Health Initiative, failed to demonstrate any reduction in breast cancer incidence with reduction in fat intake.[16] Another randomized trial, the Nurses' Health Study II, found increased breast cancer incidence in premenopausal women only, with higher intake of animal fat, but not vegetable fat. Taken as a whole, these results point to a possible association between dietary fat intake and breast cancer incidence, though these interactions are hard to measure in large groups of women.
A significant environmental effect is likely responsible for the different rates of breast cancer incidence between countries with different dietary customs. Researchers have long measured that breast cancer rates in an immigrant population soon come to resemble the rates of the host country after a few generations. The reason for this is speculated to be immigrant uptake of the host country diet. The prototypical example of this phenomenon is the changing rate of breast cancer after the arrival of Japanese immigrants to America.Template:Fact
Alcohol
Alcohol appears to increase the risk of breast cancer, though meaningful increases are limited to higher alcohol intake levels. Breast cancer constitutes about 7.3% of all cancers.[17] Among women, breast cancer comprises 60% of alcohol-attributable cancers.[18] The UK's Review of Alcohol: Association with Breast Cancer concludes that "studies confirm previous observations that there appears to be an association between alcohol intake and increased risk of breast cancer in women. On balance, there was a weak association between the amount of alcohol consumed and the relative risk."[19]
The National Institute on Alcohol Abuse and Alcoholism (NIAAA) concludes that "Chronic alcohol consumption has been associated with a small (averaging 10 percent) increase in a woman's risk of breast cancer."[20][21][22][23] According to these studies, the risk appears to increase as the quantity and duration of alcohol consumption increases. Other studies, however, have found no evidence of such a link.[24][25][26]
The Committee on Carcinogenicity of Chemicals in Food, Consumer Products Non-Technical Summary concludes, "the new research estimates that a woman drinking an average of two units of alcohol per day has a lifetime risk of developing breast cancer 8% higher than a woman who drinks an average of one unit of alcohol per day.[27] The risk of breast cancer further increases with each additional drink consumed per day. The research also concludes that approximately 6% (between 3.2% and 8.8%) of breast cancers reported in the UK each year could be prevented if drinking was reduced to a very low level (i.e. less than 1 unit/week)." A review article from JAMA also found that breast cancer incidence seems to increase with increasing alcohol consumption.[28] It has been reported that "two drinks daily increase the risk of getting breast cancer by about 25 percent" (NCI), but the evidence is inconsistent. The Framingham study has carefully tracked individuals since the 1940s. Data from that research found that drinking alcohol moderately did not increase breast cancer risk (Wellness Facts). Similarly, research by the Danish National Institute for Public Health found that moderate drinking had virtually no effect on breast cancer risk.[29]
One study suggests that women who frequently drink red wine may have an increased risk of developing breast cancer.[30]
"Folate intake counteracts breast cancer risk associated with alcohol consumption"[31] and "women who drink alcohol and have a high folate intake are not at increased risk of cancer."[32] Those who have a high (200 micrograms or more per day) level of folate (folic acid or Vitamin B9) in their diet are not at increased risk of breast cancer compared to those who abstain from alcohol.[33] Foods rich in folate include citrus fruits, citrus juices, dark green leafy vegetables (such as spinach), dried beans, and peas. Vitamin B9 can also be taken in a multivitamin pill.
Obesity
Gaining weight after menopause can increase a woman's risk. A recent study found that putting on 9.9kg (22lbs) after menopause increased the risk of developing breast cancer by 18%.[34]
Hormones
Persistently increased blood levels of estrogen are associated with an increased risk of breast cancer, as are increased levels of the androgens androstenedione and testosterone (which can be directly converted by aromatase to the estrogens estrone and estradiol, respectively). Increased blood levels of progesterone are associated with a decreased risk of breast cancer in premenopausal women.[35] A number of circumstances which increase exposure to endogenous estrogens including not having children, delaying first childbirth, not breastfeeding, early menarche (the first menstrual period) and late menopause are suspected of increasing lifetime risk for developing breast cancer.[36]
Hormonal contraceptives may produce a slight increase in the risk of breast cancer diagnosis among current and recent users, but this appears to be a short-term effect. In 1996 the largest collaborative reanalysis of individual data on over 150,000 women in 54 studies of breast cancer found a relative risk (RR) of 1.24 of breast cancer diagnosis among current combined oral contraceptive pill users; 10 or more years after stopping, no difference was seen. Further, the cancers diagnosed in women who had ever used hormonal contraceptives were less advanced than those in nonusers, raising the possibility that the small excess among users was due to increased detection.[37][38] The relative risk of breast cancer diagnosis associated with current and recent use of hormonal contraceptives did not appear to vary with family history of breast cancer.[39]
Data exist from both observational and randomized clinical trials regarding the association between postmenopausal hormone replacement therapy (HRT) and breast cancer. The largest meta-analysis (1997) of data from 51 observational studies, indicated a relative risk of breast cancer of 1.35 for women who had used HRT for 5 or more years after menopause. The estrogen-plus-progestin arm of the Women's Health Initiative (WHI), a randomized controlled trial, which randomized more than 16,000 postmenopausal women to receive combined hormone therapy or placebo, was halted early (2002) because health risks exceeded benefits. One of the adverse outcomes prompting closure was a significant increase in both total and invasive breast cancers (RR = 1.24) in women randomized to receive estrogen and progestin for an average of 5 years. HRT-related breast cancers had adverse prognostic characteristics (more advanced stages and larger tumors) compared with cancers occurring in the placebo group, and HRT was also associated with a substantial increase in abnormal mammograms. Short-term use of hormones for treatment of menopausal symptoms appears to confer little or no breast cancer risk.[39]
Environmental causes
Tobacco
Most studies have not found an increased risk of breast cancer from active tobacco smoking, although a number of studies suggest an increased risk of breast cancer in both active smokers and those exposed to secondhand smoke compared to women who reported no exposure to secondhand smoke.[40]
Radiation
Women who have received high-dose ionizing radiation to the chest (for example, as treatments for other cancers) have a relative risk of breast cancer between 2.1 to 4.0.[40]
Impact of environmental estrogenic mimics
Although environmental exposures are not generally cited as risk factors for the disease (except for diet, pharmaceuticals and radiation), a substantial and growing body of evidence indicates that exposures to certain toxic chemicals and hormone-mimicking compounds including chemicals used in pesticides, cosmetics and cleaning products contribute to the development of breast cancer. A recent Canadian study concluded that female farm workers are three times more likely to have breast cancer.[41] The increasing prevalence of these substances in the environment may explain the increasing incidence of breast cancer, though direct evidence is sparse.
Dioxins
Although not well-quantified, there has long been a concern about risk associated with environmental estrogenic compounds, such as dioxins. Template:Fact
Light levels
Researchers at the National Cancer Institute and National Institute of Environmental Health Sciences have concluded a study that suggests that artificial light during the night can be a factor for breast cancer.[42]
Viral breast cancer pathogenesis research
Humans are not the only mammals prone to breast cancer. Some strains of mice, namely the house mouse (Mus domesticus) are prone to breast cancer which is caused by infection with the mouse mammary tumour virus (MMTV or "Bittner virus" for its discoverer Hans Bittner), by random insertional mutagenesis. This finding is taken to mean that a viral etiology of human breast cancer is at least possible, though there is no definitive evidence to support the claim that MMTV causes human breast cancer. For example, there may be critical differences between cancer pathogenesis in mice and people. The understanding of the role of MMTV or other viruses in human breast cancer is preliminary as of May 2007.
Factors with minimal impact on breast cancer risk
Abortion
Studies in rats[43] led to speculation that abortion may increase the risk of breast cancer because of hormones initiating breast tissue growth in early pregnancy. Some early interview based case-control studies indicated a possible correlation,[44] but more recent large record based studies and meta-analysis studies do not support this association.[45][46] The relationship of breast cancer and abortion is the subject of a Wikipedia article called Abortion-breast cancer hypothesis.
Deodorants
Much has been made of the possible contribution of aluminum-containing underarm antiperspirants to the incidence of breast cancer, since the most common location of a breast cancer is the upper outer quadrant of the breast. Aluminum salts, such as those used in anti-perspirants, have recently been classified as metalloestrogens. In research published in the Journal of Applied Toxicology, Dr. Philippa D. Darbre of the University of Reading has shown that aluminum salts increase estrogen-related gene expression in human breast cancer cells grown in the laboratory.[47][48][49] Fortunately, this in-vitro association between aluminum salts and estrogen activity does not translate into an increased risk of breast cancer in humans. The lack of association between underarm deodorants and breast cancer has been the subject of a number of research articles.[50][51]
Fertility treatments
There is no persuasive connection between fertility medications and breast cancer.[52]
Phytoestrogens and soy
Phytoestrogens such as found in soybeans have been extensively studied in animal and human in-vitro and epidemiological studies. The literature support the following conclusions:
- Plant estrogen intake, such as from soy products, in early adolescence may protect against breast cancer later in life.[53]
- Plant estrogen intake later in life is not likely to influence breast cancer incidence either positively or negatively.[54]
It seems reasonable to conclude that soybean-based phytoestrogens are not a major contributor to the incidence of breast cancer.
Prevention in high-risk individuals
Prophylactic oophorectomy
Prophylactic oophorectomy (removal of ovaries), in high-risk individuals, when child-bearing is complete, reduces the risk of developing breast cancer by 60%, as well as reducing the risk of developing ovarian cancer by 96%.[55]
Managing side effects of prophylactic oophorectomy
Non-hormonal treatments
The side effects of Oophorectomy may be alleviated by medicines other than hormonal replacement. Non-hormonal biphosphonates (such as Fosamax and Actonel) increase bone strength and are available as once-a-week pills. Low-dose Selective Serotonin Reuptake Inhibitors (e.g. Paxil, Prozac) alleviate vasomotor menopausal symptoms, i.e. "hot flashes".[56]
Hormonal treatments
Short-term hormone replacement with estrogen, in high-risk BRCA mutation carriers, was not shown to increase the risk of breast cancer in women who are post-oophorectomy. The results were published in JCO in 2004, and the conclusions based on a computerized simulation using models of risk and benefit, a lower level of data than a randomized trial per se. PMID: 14981106. This result can probably be generalized to other women at high risk, in whom short term (i.e., one or two year) treatment with estrogen for hot flashes, may be acceptable.
Prophylactic mastectomy
Bilateral prophylactic mastectomies have been shown to prevent breast cancer in high-risk individuals, such as patients with BRCA1 or BRCA2 gene mutations.
Medications
Hormonal therapy has been used for chemoprevention in individuals at high risk for breast cancer. In 2002, a clinical practice guideline by the U.S. Preventive Services Task Force (USPSTF) recommended "clinicians discuss chemoprevention with women at high risk for breast cancer and at low risk for adverse effects of chemoprevention" with a grade B recommendation.[57][58]
Selective estrogen receptor modulators (SERMs)
The guidelines were based on studies of SERMs from the MORE, BCPT P-1, and Italian trials. In the MORE trial, the relative risk reduction for raloxifene was 76%.[59] The P-1 preventative study demonstrated that tamoxifen can prevent breast cancer in high-risk individuals. The relative risk reduction was up to 50% of new breast cancers, though the cancers prevented were more likely estrogen-receptor positive (this is analogous to the effect of finasteride on the prevention of prostate cancer, in which only low-grade prostate cancers were prevented).[60][61] The Italian trial showed benefit from tamoxifen.[62]
Additional randomized controlled trials have been published since the guidelines. The IBIS trial found benefit from tamoxifen. [63]In 2006, the NSABP STAR trial demonstrated that raloxifene had equal efficacy in preventing breast cancer compared with tamoxifen, but that there were fewer side effects with raloxifene.[64] The RUTH Trial concluded that "benefits of raloxifene in reducing the risks of invasive breast cancer and vertebral fracture should be weighed against the increased risks of venous thromboembolism and fatal stroke".[65]
Raloxifene is only FDA-approved for osteoporosis as of May 2007.
Aromatase inhibitors
Aromatase inhibitors may prove to prevent breast cancer.
Screening
X-ray mammography
Due to the high incidence of breast cancer among older women, screening is now recommended in many countries. Screening methods suggested include breast self-examination and mammography. Mammography has been estimated to reduce breast cancer-related mortality by 20-30%.[66] Routine (annual) mammography of women older than forty or fifty years of age is recommended by numerous organizations as a screening method to diagnose early breast cancer, and has demonstrated a protective effect in multiple clinical trials.[67] The evidence in favor of mammographic screening comes from eight randomized clinical trials from the 1960s through 1980s. Many of these trials have been criticised for methodological errors, and the results were summarized in a review article published in 1993.[68]
Improvements in mortality due to screening are hard to measure; similar difficulty exists in measuring the impact of Pap smear testing on cervical cancer, though worldwide, the impact of that test is likely enormous. Nationwide mortality due to cancer before and after the institution of a screening test is a surrogate indicator about the effectiveness of screening, and results of mammography are favorable.
The U.S. National Cancer Institute recommends screening mammography with a baseline mammogram at age 35, mammograms every two years beginning at age 40, and then annual mammograms beginning at age 50. In the UK, women are invited to attend for screening once every three years beginning at age 50. Women with one or more first-degree relatives (mother, sister, daughter) with premenopausal breast cancer should begin screening at an earlier age. It is usually suggested to start screening at an age that is 10 years less than the age at which the relative was diagnosed with breast cancer. More and more men are being prompted to undertake breast screening due to the rise of breast cancer in men.Template:Fact
Part of the difficulty in interpreting mammograms in younger women stems from the problem of breast density. Radiographically, a dense breast has a preponderance of glandular tissue, and younger age or estrogen hormone replacement therapy contribute to mammographic breast density. After menopause, the breast glandular tissue gradually is replaced by fatty tissue, making mammographic interpretation much more accurate. Some authors speculate that part of the contribution of estrogen hormone replacement therapy to breast cancer mortality arises from the issue of increased mammographic breast density. Breast density is an independent adverse prognostic factor on breast cancer prognosis.
Several scientific groups however have expressed concern on the perceived benefits of breast screening by the public.[69] In 2001, a controversial review published in The Lancet claimed that there is no reliable evidence that screening for breast cancer reduces mortality.[70] The results of this study were widely reported in the popular press.[71]
False positives are a major problem of mammographic breast cancer screening. Data reported in the UK Million Woman Study indicates that if 134 mammograms are performed, 20 women will be called back for suspicious findings, four biopsies will be necessary, to diagnose one cancer. Recall rates are higher in the USA than in the UK.[72] The contribution of mammography to the early diagnosis of cancer cannot be overstated, but it comes at a huge financial and psychological cost to the women found to have a nodule.
In general, digital mammography and computer-aided mammography have increased the sensitivity of mammograms, but at the cost of more numerous false positive results.
Mammography is still the modality of choice for screening of early breast cancer, since it is relatively fast, reasonably accurate, and widely available in developed countries. Breast cancers detected by mammography are usually much smaller (earlier stage) than those detected by patients or doctors as a breast lump.
Breast MRI
Magnetic resonance imaging (MRI) has been shown to detect cancers that are not visible on mammograms, but it has several disadvantages. For example, although it is 27-36% more sensitive, it is less specific than mammography.[73] As a result, MRI studies will have more false positives (up to 5%), which may have undesirable financial and psychological costs. It is also a relatively expensive procedure, and one which requires the intravenous injection of a chemical agent to be effective. Proposed Indications for using MRI for screening include:[74]
- Strong family history of breast cancer
- Patients with BRCA-1 or BRCA-2 oncogene mutations
- Evaluation of women with breast implants
- History of previous lumpectomy or breast biopsy surgeries
- Axillary metastasis with an unknown primary tumor
- Very dense or scarred breast tissue
Breast ultrasound
Ultrasound alone is not usually employed as a screening tool but it is a useful additional tool for the characterization of palpable tumours and directing image-guided biopsies. U-Systems is a US-based company that is selling a breast-cancer detection system using ultrasound that is fully-automated. Using an ultrasound allows a look at dense breast tissue which is not possible with digital mammmography. It is closely correlated with the digital mammography. The other significant advantage over digital mammography is that it is a pain-free procedure.
Breast self-exam
Breast self-exam was widely discussed in the 1990s as a useful modality for detecting breast cancer at an earlier stage of presentation. A large clinical trial in China reduced enthusiasm for breast self-exam. In the trial, reported in the Journal of the National Cancer Institute first in 1997 and updated in 2002, 132,979 female Chinese factory workers were taught breast self-exam monthly by nurses at their factories, while 133,085 other workers were not taught self-exam. The women taught self-exam tended to detect more breast nodules, but breast cancer mortality was no different from the control women. In other words, women taught breast self-exam were mostly likely to detect benign breast disease, but were just as likely to die of breast cancer. [75]An editorial in the Journal of the National Cancer Institute reported in 2002, "Routinely Teaching Breast Self-Examination is Dead. What Does This Mean?" [76]
Diagnosis
The diagnosis of breast cancer is established by the pathological (microscopic)examination of surgically removed breast tissue. A number of procedures can obtain tissue or cells prior to definitive treatment for histological or cytological examination. Such procedures include fine-needle aspiration, nipple aspirates, ductal lavage, core needle biopsy, and local surgical excisional biopsy. These diagnostic steps, when coupled with radiographic imaging, are usually accurate in diagnosing a breast lesion as cancer. Occasionally, pre-surgical procedures such as fine needle aspirate may not yield enough tissue to make a diagnosis, or may miss the cancer entirely. Imaging tests are sometimes used to detect metastasis and include chest x-ray, bone scan, CT, MRI, and PET scanning. While imaging studies are useful in determining the presence of metastatic disease, they are not in and of themselves diagnostic of cancer. Only microscopic evaluation of a biopsy specimen can yield a cancer diagnosis. Ca 15.3 (carbohydrate antigen 15.3, epithelial mucin) is a tumor marker determined in blood which can be used to follow disease activity over time after definitive treatment. Blood tumor marker testing is not routinely performed for the screening of breast cancer, and has poor performance characteristics for this purpose.
Staging
Breast cancer is staged according to the TNM system, updated in the AJCC Staging Manual, now on its sixth edition. Prognosis is closely linked to results of staging, and staging is also used to allocate patients to treatments both in clinical trials and clinical practice.
Summary of stages:
- Stage 0 - Carcinoma in situ
- Stage I - Tumor (T) does not exceed 2 cm, no axillary lymph nodes (N) involved.
- Stage IIA – T 2-5 cm, N negative, or T <2 cm and N positive.
- Stage IIB – T > 5 cm, N negative, or T 2-5 cm and N positive (< 4 axillary nodes).
- Stage IIIA – T > 5 cm, N positive, or T 2-5 cm with 4 or more axillary nodes
- Stage IIIB – T has penetrated chest wall or skin, and may have spread to < 10 axillary N
- Stage IIIC – T has > 10 axillary N, 1 or more supraclavicular or infraclavicular N, or internal mammary N.
- Stage IV – Distant metastasis (M)
Breast lesions are examined for certain markers, notably sex steroid hormone receptors. About two thirds of postmenopausal breast cancers are estrogen receptor positive (ER+) and progesterone receptor positive (PR+).[77] Receptor status modifies the treatment as, for instance, only ER-positive tumors, not ER-negative tumors, are sensitive to hormonal therapy.
The breast cancer is also usually tested for the presence of human epidermal growth factor receptor 2, a protein also known as HER2, neu or erbB2. HER2 is a cell-surface protein involved in cell development. In normal cells, HER2 controls aspects of cell growth and division. When activated in cancer cells, HER2 accelerates tumor formation. About 20-30% of breast cancers overexpress HER2. Those patients may be candidates for the drug Herceptin, both in the postsurgical setting (so-called "adjuvant" therapy), and in the metastatic setting.[78]
Treatment personalization with gene expression profiling
Recently, the acceleration of gene expression profiling research has made available additional markers to predict disease recurrence. Beyond conventional TNM staging, doctors can now order a gene expression profile on tumors to predict whether a breast cancer patient will have a high chance of developing breast cancer again. The test, Oncotype-DX, is not used in every clinical setting; for example, in a patient with positive lymph nodes who is a candidate for chemotherapy, the test would not change therapy decisions. The most useful setting for Oncotype-DX testing is where there are negative lymph nodes, and the benefit of chemotherapy is felt to be small. In up to 10% of patients, there will be disease recurrences, but treating every patient with chemotherapy is overkill. In this setting, a high-risk score on the Oncotype-DX can help doctors decide whether to recommend chemotherapy.
Treatment
The mainstay of breast cancer treatment is surgery when the tumor is localized, with possible adjuvant hormonal therapy (with tamoxifen or an aromatase inhibitor), chemotherapy, and/or radiotherapy. At present, the treatment recommendations after surgery (adjuvant therapy) follow a pattern. This pattern is subject to change as every two years a worldwide conference takes place in St. Gallen, Switzerland to discuss the actual results of worldwide multi-center studies. Depending on clinical criteria (age, type of cancer, size, metastasis) patients are roughly divided to high risk and low risk cases which follow different rules for therapy. Treatment possibilities include Radiation Therapy, Chemotherapy, Hormone Therapy, and Immune Therapy.
An online resource for helping to quantify the relative risks and benefits of chemotherapy and hormonal therapy is Adjuvant! Online (see below).
In planning treatment, doctors can also use PCR tests like Oncotype DX or microarray tests like MammaPrint that predict breast cancer recurrence risk based on gene expression. In February 2006, the MammaPrint test became the first breast cancer predictor to win formal approval from the Food and Drug Administration. This is a new gene test to help predict whether women with early stage breast cancer will relapse in five or 10 years, this could help influence how aggressively they fight the initial tumor.[79]
Surgery
Depending on the staging and type of the tumor, just a lumpectomy (removal of the lump only) may be all that is necessary or removal of larger amounts of breast tissue may be necessary. Surgical removal of the entire breast is called mastectomy.
While there has been an increasing utilization of lumpectomy techniques for breast-conservation cancer surgery, mastectomy may be the preferred treatment in certain instances:
- Two or more tumors exist in different areas of the breast (a "multifocal" cancer).
- The breast has previously received radiation (XRT) treatment.
- The tumor is large relative to the size of the breast.
- The patient has had scleroderma or another disease of the connective tissue, which can complicate XRT treatment.
- The patient lives in an area where XRT is inaccessible.
- The patient is apprehensive about their risk of local recurrence after lumpectomy.
Standard practice requires the surgeon to establish that the tissue removed in the operation has margins clear of cancer, indicating that the cancer has been completely excised. If the tissue removed does not have clear margins, then further operations to remove more tissue may be necessary. This may sometimes require removal of part of the pectoralis major muscle which is the main muscle of the anterior chest wall.
During the operation, the lymph nodes in the axilla are also considered for removal. In the past, large axillary operations took out ten to forty nodes to establish whether cancer had spread. This had the unfortunate side effect of frequently causing lymphedema of the arm on the same side, as the removal of this many lymph nodes affected lymphatic drainage. More recently, the technique of sentinel lymph node (SLN) dissection has become popular, as it requires the removal of far fewer lymph nodes, resulting in fewer side effects. The sentinel lymph node is the first node that drains the tumor, and subsequent SLN mapping can save 65-70% of patients with breast cancer from having a complete lymph node dissection for what could turn out to be a negative nodal basin. Advances in Sentinel Lymph Node mapping over the past decade have increased the accuracy of detecting Sentinel Lymph Node from 80% using blue dye alone to between 92% and 98% using combined modalities.[80] SLN biopsy is indicated for patients with T1 and T2 lesions (<5cm) and carries a number of recommendations for use on patient subgroups.[80]
Radiation therapy
Radiation therapy consists of the use of high powered X-rays or gamma rays (XRT) that precisely target the area that is being treated. These X-rays or gamma rays are very effective in destroying the cancer cells that might recur where the tumor was removed. These X-rays are delivered by a machine called a linear Accelerator or LINAC. Alternatively, the use of implanted radioactive catheters (brachytherapy), similar to those used in prostate cancer treatment, is being evaluated. The use of radiation therapy for breast cancer is usually given after surgery has been performed and is an essential component of breast conserving therapy. The purpose of radiation is to reduce the chance that the cancer will recur.
Radiation therapy works for breast cancer by eliminating the microscopic cancer cells that may remain near the area where the tumor was removed during surgery. Since by the nature of radiation and its effects on normal cells and cancer cells alike the dose that is given is to ensure that the cancer cells are eliminated. However, the dose cannot be given in one sitting. Radiation causes some damage to the normal tissue around where the tumor was but normal healthy tissue can repair itself. The treatments are given typically over a period of five to seven weeks, performed five days a week. Each treatment session takes about fifteen minutes per day. Breaking the treatments up over this extended period of time gives the healthy normal tissue a chance to repair itself. Cancer cells do not repair themselves as well as normal cells, which explains the efficacy of radiation therapy.
Although radiation therapy can reduce the chance that breast cancer will recur in the breast, it is much less effective in prolonging patient survival. The National Cancer Institute reviews this information.[81] in a paragraph that begins:“Breast-conserving surgery alone without radiation therapy . . .” The NCI includes six studies; none of them found a survival benefit for radiation therapy. Abstracts from all six studies are available for review. Patients who are unable to have radiation therapy after lumpectomy should consult with a surgeon who understands this research and who believes that lumpectomy (or partial mastectomy) alone is a reasonable treatment option.
Indications for radiation
Indications for radiation treatment are constantly evolving. Patients treated in Europe have been more likely in the past to be recommended adjuvant radiation after breast cancer surgery. Radiation therapy is usually recommended for all patients who had (lumpectomy, quadrant-resection). Radiation therapy is usually not indicated in patients with advanced (stage IV disease) except for palliation of symptoms like bone pain.
In general recommendations would include:
- As part of breast conserving therapy of breast cancer when the whole breast is not removed (lumpectomy or wide local excision)
- After mastectomy: Patients with higher chances of cancer recurring such as : large primary tumor and involvement of 4 or more lymph nodes.
Other factors which may influence adding adjuvant radiation therapy:
- Tumor close to or involving the margins on pathology specimen
- Multiple areas of tumor (multicentric disease)
- Microscopic invasion of lymphatic or vascular tissues
- Microcopic invasion of the skin, nipple/areola, or underlying pectoralis major muscle
- Patients with <4 LN involved, but extension out of the substance of a LN
- Inadequate numbers of axillary LN sampled
Types of radiotherapy
Radiotherapy can be delivered in many ways. Most commonly this is done using radiation from linear accelerators. Since this is delivered from outside, one needs to restrict the amount of dose that can be given at one time so that normal tissues are not harmed. So the course usually lasts for several days, typically every day for 5 to 6 weeks.
New technology has allowed more precise delivery of radiotherapy in a portable fashion - for example in the operating theatre. Targeted intraoperative radiotherapy (TARGIT).[82] is a method of delivering therapeutic radiation from within the breast using a portable x-ray generator called Intrabeam. It is undergoing clinical trials in several countries at present to test whether it can replace the whole course of radiotherapy in selected patients.[83] It may also be able provide a much better boost dose to the tumour bed and appears to provide superior control.[84] This will be tested in a Targit-B trial.[85]
Side effects of radiation therapy
The side effects of radiation have decreased considerably over the past decades. Aside from general fatigue caused by the healthy tissue repairing itself, there will probably be no side effects at all. Some patients develop a suntan-like change in skin color in the exact area being treated. As with a suntan, this darkening of the skin will fade with time. Other side effects experienced with radiation include the fact that radiation therapy can and often does cause permanent changes in the color and texture of skin, in addition to:
- reddening of the skin
- muscle stiffness
- mild swelling
- tenderness in the area
- long-term shrinking of the irradiated breast
Along with improved cosmetic outcome of treatment with radiation, there have been improvements in the techniques that deliver radiation to the breast. One such new technology is using IMRT (intensity modulated radiation therapy), in which the radiation oncologist can change the shape and intensity of the radiation beam at different points across and inside the breast. This allows for a more focused beam of radiation directed at the tumor cells and leaves most of the healthy tissue unaffected by the radiation.
Another new procedure involves a type of brachytherapy, where a radioactive source is temporarily placed inside the breast in direct contact with the tumor bed (area where tumor was removed). This technique is called a Mammosite and is currently undergoing clinic trials.
The use of adjuvant radiation has significant potential effects if the patient has to later undergo breast reconstruction surgery. Fibrosis of chest wall skin from radiation negatively affects skin elasticity and makes tissue expansion techniques difficult. Traditionally most patients are advised to defer immediate breast reconstruction when adjuvant radiation is planned and are most often recommended surgery involving autologous tissue reconstruction rather then breast implants.
Systemic therapy
Systemic therapy uses medications to treat cancer cells throughout the body. Any combination of systemic treatments may be used to treat breast cancer. Systemic treatments include chemotherapy, immune therapy, and hormonal therapy.
Chemotherapy
Chemotherapy (drug treatment for cancer) may used before surgery, after surgery, or instead of surgery in those patients who are unsuitable for surgery.
See breast cancer chemotherapy.
Hormonal treatment
Patients with estrogen receptor positive tumors will typically receive a hormonal treatment after chemotherapy is completed. Typical hormonal treatments include:
- Tamoxifen is typically given to premenopausal women to inhibit the estrogen receptors
- Aromatase inhibitors are typically given to postmenopausal women to lower the amount of estrogen in their systems
- GnRH-analogues
- ovarian ablation or suppression is used in premenopausal women
Targeted therapy
In patients whose cancer expresses an over-abundance of the HER2 protein, a monoclonal antibody known as trastuzumab (Herceptin ®) is used to block the activity of the HER2 protein in breast cancer cells, slowing their growth. This drug was originally used only in the treatment of patients with metastatic disease, however in the summer of 2005 two large clinical trials published results suggesting that patients with early-stage disease also benefit significantly from Herceptin. The drug was approved by the FDA in 1998 for the treatment of metastatic breast cancer, though oncologists have also been using it since 2005 for postoperative patients with localized, Her-2/neu positive disease.
Antiangiogenic therapy
A commercially-available monoclonal antibody that blocks the activation of the VEGF receptor, bevacizumab, underwent testing in a randomized clinical trial in patients with metastatic breast cancer. Bevacizumab has improved overall survival in both lung cancer and colon cancer by blocking the growth of new blood vessels around tumors, and by improving the permeability profile of tumor blood vessels to enhance the delivery of chemotherapy to the tumor. Results were presented in abstract form at the San Antonio Breast Cancer Meeting in 2005 and updated in 2006. There has been no formal publication of the data in the peer-reviewed literature as of May, 2007. The data indicate that bevacizumab delays disease progression for up to five months over conventional chemotherapy, but survival was no better. Genentech, manufacturer of bevacizumab, has filed a supplemental biological application with the FDA for approval of bevacizumab in the setting of metastatic breast cancer, on the strength of the improvement in progression-free survival.
Preclinical
PTPB1
In the May 12 2007, edition of the scientific journal, Nature Genetics, researchers from Canada's McGill University reported that they have developed a potential drug target for treating up to 40 percent of breast cancers by blocking an enzyme called PTPB1, which has been implicated in the onset of breast cancer in mouse models of the disease. Elevated levels of PTPB1 have also been found in diabetes and obesity. A drug to block the activity of PTPB1 is under development by Merck, and was found to delay the development of breast tumors and prevent lung cancer up to two months from the administration of the drug. The researchers hope to continue further research in mouse models which are also HER-2 positive (responsive to Herceptin) so that the drug could benefit a significant population of women.[86]
Flax seeds
Preliminary research into flax seeds indicate that flax can significantly inhibit breast cancer growth and metastasis, and enhance the inhibitory effect of tamoxifen on estrogen-dependent tumors.[87][88][89][90]
Traditional Chinese medicine
The use of traditional Chinese medicine to treat breast cancer has been claimed, but no successful clinical trials have yet been reported.
Psychological aspects of breast cancer diagnosis and treatment
The emotional impact of cancer diagnosis, symptoms, treatment, and related issues can be severe. Most larger hospitals are associated with cancer support groups which can help patients cope with the many issues that come up in a supportive environment with other people with experience with similar issues. Online cancer support groups are also very beneficial to cancer patients, especially in dealing with uncertainty and body-image problems inherent in cancer treatment.
Prognosis
There are several prognostic factors associated with breast cancer. Stage is the single most important prognostic factor in breast cancer, as it will take into consideration local involvement, lymph node status and whether metastatic disease is present or not. The higher the stage at the time of diagnosis, the worse the prognosis of breast cancer is. Node negative breast cancer patients have a much better prognosis compared to node positive patients.
Presence of estrogen and progesterone receptors in the cancer cell is another important prognostic factor, and may guide treatment. Hormone receptor positive breast cancer is usually associated with much better prognosis compared to hormone negative breast cancer.
HER2/neu status has also been described as a prognostic factor. Patients whose cancer cells are positive for HER2/neu have more aggressive disease and may be treated with trastuzumab, a monoclonal antibody that targets this protein.
Ashkenazi Jewish women and black women tend to have higher rates of fatalities.Template:Fact
Breast cancer in males
Less than 1% of breast cancers occur in men, and incidence is about 1 in 100,000. Men with gynaecomastia do not have a higher risk of developing breast cancer.[91] There may be an increased incidence of breast cancer in men with prostate cancer. The prognosis, even in stage I cases, is worse in men than in women.[92] The treatment of men with breast cancer is similar to that in older women. Since the male breast tissue is confined to the area directly behind the nipple, treatment for males has usually been a mastectomy with axillary surgery. This may be followed by adjuvant radiotherapy, hormone therapy (such as tamoxifen), or chemotherapy.
Breast cancer metastasis
Most people understand breast cancer as something that happens in the breast. However it can metastasise (spread) via lymphatics to nearby lymph nodes usually those under the arm. That is why surgery for breast cancer always involves some type of surgery for the glands under the arm- either axillary clearance, sampling or sentinel node biopsy.
Breast cancer can also spread to other parts of the body via blood vessels. So it can spread to the lungs, pleura (the lining of the lungs), the liver, the brain and most commonly to the bones.
Seventy percent of the time that breast cancer spreads to other locations, it spreads to bone, especially the vertebrae and the long bones of the arms, legs and ribs. Breast cancer cells "set up house" in the bones and form tumors. When breast cancer is found in bones, it has usually spread to more than one site. At this stage, it is treatable, often for many years, but it is not curable.
Like normal breast cells, these tumors in the bone often thrive on female hormones, especially estrogen. Therefore, the doctor often treats the patient with medicines that lower her estrogen levels.
Usually when breast cancer spreads to bone, it eats away healthy bone causing weak spots. The bones break easily at these weak spots. That is why breast cancer patients are often seen wearing braces or using a wheel chair, and why they complain about aching bones. If a patient has had breast cancer in the past and notices pain in the bones, the patient should see a doctor.Template:Fact
Breast cancer awareness
In the month of October, breast cancer is recognized by survivors, family and friends of survivors and/or victims of the disease. A pink ribbon is worn to recognize the struggle that sufferers face when battling the cancer.
Pink for October is an initiative started by Matthew Oliphant, which asks that any sites willing to help make people aware of breast cancer, change their template or layout to include the color pink, so that when visitors view the site, they see that the majority of the site is pink. Then after reading a short amount of information about breast cancer, or being redirected to another site, they are aware of the disease itself.
See also
- List of notable breast cancer patients according to occupation
- List of notable breast cancer patients according to survival status
- List of breast carcinogenic substances
- Mammary tumor for breast cancer in other animals
- Breast reconstruction
- Alcohol and cancer
- Mammography Quality Standards Act
- National Breast Cancer Coalition
- Breast Cancer Action
- Barron Lerner (Physician)
- William Stewart Halsted (Radical Masectomy)
References
- ↑ 1.0 1.1 WHO (February 2006). Fact sheet No. 297: Cancer. Retrieved on 2007-04-26.
- ↑ American Cancer Society (2007). Cancer Facts & Figures 2007. Retrieved on 2007-04-26.
- ↑ 3.0 3.1 American Cancer Society (2006-09-18). What Are the Key Statistics for Breast Cancer?. Retrieved on 2007-05-22.
- ↑ Laurance, Jeremy. Breast cancer cases rise 80% since Seventies, The Independent, 2006-09-29. Retrieved on 2006-10-09.
- ↑ Breast Cancer: Statistics on Incidence, Survival, and Screening. Imaginis Corporation (2006). Retrieved on 2006-10-09.
- ↑ Male Breast Cancer Treatment - National Cancer Institute. National Cancer Institute (2006). Retrieved on 2006-10-16.
- ↑ Breast Cancer: Molecular Genetics, Pathogenesis, and Therapeutics (Contemporary Cancer Research) by Anne M. Bowcock (1999)
- ↑ The History of Cancer. American Cancer Society (2002-03-25). Retrieved on 2006-10-09.
- ↑ Cavalieri E, Chakravarti D, Guttenplan J, et al (2006). "Catechol estrogen quinones as initiators of breast and other human cancers: implications for biomarkers of susceptibility and cancer prevention". Biochim. Biophys. Acta 1766 (1): 63-78. DOI:10.1016/j.bbcan.2006.03.001. PMID 16675129. Research Blogging.
- ↑ Madigan MP, Ziegler RG, Benichou J, Byrne C, Hoover RN (1995). "Proportion of breast cancer cases in the United States explained by well-established risk factors". J. Natl. Cancer Inst. 87 (22): 1681-5. PMID 7473816. Retrieved on 2007-05-26. [e]
- ↑ Individual Risk Factors. BreastCander.org. Retrieved on 2007-03-11.
- ↑ Giordano, Sharon H; Cohen DS, Buzdar AU, Perkins G, Hortobagyi GN (May 2004). "Breast carcinoma in men". Cancer 101 (1): 51-57. [e]
- ↑ 13.0 13.1 Malone KE, Daling JR, Thompson JD, O'Brien CA, Francisco LV, Ostrander EA (1998). "BRCA1 mutations and breast cancer in the general population: analyses in women before age 35 years and in women before age 45 years with first-degree family history". JAMA 279 (12): 922-9. PMID 9544766. [e]
- ↑ Chlebowski RT, Blackburn GL, Thomson CA, Nixon DW, Shapiro A, Hoy MK, et al.. "Dietary fat reduction and breast cancer outcome: interim efficacy results from the Women's Intervention Nutrition Study (WINS).". J Natl Cancer Inst 98 (24): 1767-1776. PMID 17179478.
- ↑ Hunter DJ, Spiegelman D, Adami HO, et al (1996). "Cohort studies of fat intake and the risk of breast cancer--a pooled analysis". N. Engl. J. Med. 334 (6): 356-61. PMID 8538706. [e]
- ↑ Prentice RL, Caan B, Chlebowski RT, et al (2006). "Low-fat dietary pattern and risk of invasive breast cancer: the Women's Health Initiative Randomized Controlled Dietary Modification Trial". JAMA 295 (6): 629-42. DOI:10.1001/jama.295.6.629. PMID 16467232. Research Blogging.
- ↑ Statistics for 2007. American Cancer Society. Retrieved on 2007-03-11.
- ↑ Boffetta, Paolo; Hashibe, Mia; La Vecchia, Carlo; Zatonski, Witold; Rehm, Jürgen (2006-03-23). "The burden of cancer attributable to alcohol drinking". International Journal of Cancer 119 (4): 884–887. DOI:10.1002/ijc.21903. PMID 16557583. Retrieved on 2006-10-09. Research Blogging.
- ↑ Review of Alcohol: Association with Breast Cancer. U.K. Dept. of Health. Retrieved on 2007-03-11.
- ↑ Friedenreich C, Howe G, Miller A, Jain M (1993). "A cohort study of alcohol consumption and risk of breast cancer". Am J Epidemiol 137 (5): 512-20. PMID 8465803.
- ↑ Longnecker M, Berlin J, Orza M, Chalmers T (1988). "A meta-analysis of alcohol consumption in relation to risk of breast cancer". JAMA 260 (5): 652-6. PMID 3392790.
- ↑ Longnecker MP (1992). "Alcohol consumption in relation to risk of cancers of the breast and large bowel". Alcohol Health & Research World 16 (3): 223-229.
- ↑ Nasca P, Baptiste M, Field N, Metzger B, Black M, Kwon C, Jacobson H (1990). "An epidemiological case-control study of breast cancer and alcohol consumption". Int J Epidemiol 19 (3): 532-8. PMID 2262245.
- ↑ Chu S, Lee N, Wingo P, Webster L (1989). "Alcohol consumption and the risk of breast cancer". Am J Epidemiol 130 (5): 867-77. PMID 2683749.
- ↑ Schatzkin A, Piantadosi S, Miccozzi M, Bartee D (1989). "Alcohol consumption and breast cancer: a cross-national correlation study". Int J Epidemiol 18 (1): 28-31. PMID 2722377.
- ↑ Webster L, Layde P, Wingo P, Ory H (1983). "Alcohol consumption and risk of breast cancer". Lancet 2 (8352): 724-6. PMID 6136850.
- ↑ CONSUMPTION OF ALCOHOLIC BEVERAGES AND RISK OF BREAST CANCER IN WOMEN. U.K. Dept. of Health. Retrieved on 2007-03-11.
- ↑ Singletary KW, Gapstur SM (2001). "Alcohol and breast cancer: review of epidemiologic and experimental evidence and potential mechanisms". JAMA 286 (17): 2143-51. PMID 11694156. [e]
- ↑ Petri A, Tjønneland A, Gamborg M, Johansen D, Høidrup S, Sørensen T, Grønbaek M (2004). "Alcohol intake, type of beverage, and risk of breast cancer in pre- and postmenopausal women". Alcohol Clin Exp Res 28 (7): 1084-90. PMID 15252295.
- ↑ Maggiolini M, Recchia A, Bonofiglio D, Catalano S, Vivacqua A, Carpino A, Rago V, Rossi R, Andò S (2005). "The red wine phenolics piceatannol and myricetin act as agonists for estrogen receptor alpha in human breast cancer cells". J Mol Endocrinol 35 (2): 269-81. PMID 16216908.
- ↑ Mayo Clinic news release June 26 2001 "Folate Intake Counteracts Breast Cancer Risk Associated with Alcohol Consumption"
- ↑ Boston University Folate, Alcohol, and Cancer Risk
- ↑ Zhang S, Hunter D, Hankinson S, Giovannucci E, Rosner B, Colditz G, Speizer F, Willett W (1999). "A prospective study of folate intake and the risk of breast cancer". JAMA 281 (17): 1632-7. PMID 10235158.
- ↑ BBC report Weight link to breast cancer risk
- ↑ Yager JD; Davidson NE (2006). "Estrogen carcinogenesis in breast cancer". New Engl J Med 354 (3): 270-82. PMID 16421368.
- ↑ American Cancer Society. (2006-10-03). What Are the Risk Factors for Breast Cancer? Retrieved 2006-03-30.
- ↑ Collaborative Group on Hormonal Factors in Breast Cancer (1996). "Breast cancer and hormonal contraceptives: collaborative reanalysis of individual data on 53,297 women with breast cancer and 100,239 women without breast cancer from 54 epidemiological studies". Lancet 347 (9017): 1713-27. PMID 8656904.
- ↑ Collaborative Group on Hormonal Factors in Breast Cancer (1996). "Breast cancer and hormonal contraceptives: further results". Contraception 54 (3 Suppl): 1S-106S. PMID 8899264.
- ↑ 39.0 39.1 National Cancer Institute (2006-08-03). Hormone Therapy. Genetics of Breast and Ovarian Cancer. Retrieved on 2006-08-12.
- ↑ 40.0 40.1 ACS (2005). Breast Cancer Facts & Figures 2005-2006. Retrieved on 2007-04-26.
- ↑ Ctv.Ca News Staff. Breast cancer more likely in farm workers: study, Ctv.Ca, 2006-10-12. Retrieved on 2007-03-11.
- ↑ The Independent Avoid breast cancer. Sleep in the dark...
- ↑ Russo J, Russo I (1987). "Biological and molecular bases of mammary carcinogenesis". Lab Invest 57 (2): 112-37. PMID 3302534.
- ↑ Daling J.R. et al. (1994) PubMed Risk of breast cancer among young women: relationship to induced abortion. J Natl Cancer Inst. 1994 Nov 2;86(21):1584-92.
- ↑ Melbye M, Wohlfahrt J, Olsen J, Frisch M, Westergaard T, Helweg-Larsen K, Andersen P (1997). "Induced abortion and the risk of breast cancer". N Engl J Med 336 (2): 81-5. PMID 8988884.
- ↑ Beral V, Bull D et al, "Breast cancer and abortion: collaborative reanalysis of data from 53 epidemiological studies, including 83,000 women with breast cancer from 16 countries." Lancet, 2004 Mar 27;363(9414):1007-16 PMID 15051280
- ↑ Harding, Anne. (2006) Aluminum Salts Could Increase Breast Cancer Risk. Reuters Health.
- ↑ Darbre, PD (2006). "Metalloestrogens: an emerging class of inorganic xenoestrogens with potential to add to the oestrogenic burden of the human breast.". Journal of Applied Toxicology 26 (3): 191-7. PMID 16489580.
- ↑ Darbre, PD (2005). "Aluminium, antiperspirants and breast cancer.". Journal of Inorganic Biochemistry 99 (9): 1912-9. PMID 16045991mmmmmmiii.
- ↑ Surendran A (2004). "Studies linking breast cancer to deodorants smell rotten, experts say". Nat. Med. 10 (3): 216. DOI:10.1038/nm0304-216b. PMID 14991030. Research Blogging.
- ↑ (2003) "Antiperspirants don't cause breast cancer". Harvard women's health watch 10 (5): 7. PMID 12543590. [e]
- ↑ Potashnik G, Lerner-Geva L, Genkin L, Chetrit A, Lunenfeld E, Porath A (1999). "Fertility drugs and the risk of breast and ovarian cancers: results of a long-term follow-up study". Fertil. Steril. 71 (5): 853-9. PMID 10231045. [e]
- ↑ Rice S, Whitehead SA (2006). "Phytoestrogens and breast cancer--promoters or protectors?". Endocr. Relat. Cancer 13 (4): 995-1015. DOI:10.1677/erc.1.01159. PMID 17158751. Research Blogging.
- ↑ Gikas PD, Mokbel K. (2005Phytoestrogens and the risk of breast cancer: a review of the literature. Int J Fertil Women's Med.
- ↑ Kauff N, Satagopan J, Robson M, Scheuer L, Hensley M, Hudis C, Ellis N, Boyd J, Borgen P, Barakat R, Norton L, Castiel M, Nafa K, Offit K (2002). "Risk-reducing salpingo-oophorectomy in women with a BRCA1 or BRCA2 mutation". N Engl J Med 346 (21): 1609-15. PMID 12023992.
- ↑ [1]Brigham and Women's Hospital, Boston, Massachusetts.
- ↑ (2002) "Chemoprevention of breast cancer: recommendations and rationale". Ann. Intern. Med. 137 (1): 56-8. PMID 12093249. [e]
- ↑ Kinsinger LS, Harris R, Woolf SH, Sox HC, Lohr KN (2002). "Chemoprevention of breast cancer: a summary of the evidence for the U.S. Preventive Services Task Force". Ann. Intern. Med. 137 (1): 59-69. PMID 12093250. [e]
- ↑ Cummings SR, Eckert S, Krueger KA, et al (1999). "The effect of raloxifene on risk of breast cancer in postmenopausal women: results from the MORE randomized trial. Multiple Outcomes of Raloxifene Evaluation". JAMA 281 (23): 2189-97. PMID 10376571. [e]
- ↑ Fisher B, Costantino JP, Wickerham DL, et al (2005). "Tamoxifen for the prevention of breast cancer: current status of the National Surgical Adjuvant Breast and Bowel Project P-1 study". J. Natl. Cancer Inst. 97 (22): 1652-62. DOI:10.1093/jnci/dji372. PMID 16288118. Research Blogging.
- ↑ Fisher B, Costantino JP, Wickerham DL, et al (1998). "Tamoxifen for prevention of breast cancer: report of the National Surgical Adjuvant Breast and Bowel Project P-1 Study". J. Natl. Cancer Inst. 90 (18): 1371-88. PMID 9747868. [e]
- ↑ Veronesi U, Maisonneuve P, Rotmensz N, et al (2007). "Tamoxifen for the prevention of breast cancer: late results of the Italian Randomized Tamoxifen Prevention Trial among women with hysterectomy". J. Natl. Cancer Inst. 99 (9): 727-37. DOI:10.1093/jnci/djk154. PMID 17470740. Research Blogging.
- ↑ Cuzick J, Forbes JF, Sestak I, et al (2007). "Long-term results of tamoxifen prophylaxis for breast cancer--96-month follow-up of the randomized IBIS-I trial". J. Natl. Cancer Inst. 99 (4): 272-82. DOI:10.1093/jnci/djk049. PMID 17312304. Research Blogging.
- ↑ Vogel VG, Costantino JP, Wickerham DL, et al (2006). "Effects of tamoxifen vs raloxifene on the risk of developing invasive breast cancer and other disease outcomes: the NSABP Study of Tamoxifen and Raloxifene (STAR) P-2 trial". JAMA 295 (23): 2727-41. DOI:10.1001/jama.295.23.joc60074. PMID 16754727. Research Blogging.
- ↑ Barrett-Connor E, Mosca L, Collins P, et al Raloxifene Use for The Heart (RUTH) Trial Investigators. (2006). "Effects of raloxifene on cardiovascular events and breast cancer in postmenopausal women". N. Engl. J. Med. 355 (2): 125-37. DOI:10.1056/NEJMoa062462. PMID 16837676. Research Blogging.
- ↑ Elwood J, Cox B, Richardson A. "The effectiveness of breast cancer screening by mammography in younger women.". Online J Curr Clin Trials Doc No 32: [23,227 words; 195 paragraphs]. PMID 8305999.
- ↑ Fletcher S, Black W, Harris R, Rimer B, Shapiro S (1993). "Report of the International Workshop on Screening for Breast Cancer.". J Natl Cancer Inst 85 (20): 1644-56. PMID 8105098.
- ↑ Fletcher SW, Black W, Harris R, Rimer BK, Shapiro S (1993). "Report of the International Workshop on Screening for Breast Cancer". J. Natl. Cancer Inst. 85 (20): 1644-56. PMID 8105098. Retrieved on 2007-05-26. [e]
- ↑ Women 'misjudge screening benefits', BBC, Monday, 15 October, 2001. Retrieved on 2007-04-04.
- ↑ Olsen O, Gøtzsche P (2001). "Cochrane review on screening for breast cancer with mammography". Lancet 358 (9290): 1340-2. PMID 11684218.
- ↑ New concerns over breast screening, BBC, Thursday, 18 October, 2001. Retrieved on 2007-04-04.
- ↑ Smith-Bindman R, Ballard-Barbash R, Miglioretti DL, Patnick J, Kerlikowske K (2005). "Comparing the performance of mammography screening in the USA and the UK". Journal of medical screening 12 (1): 50-4. DOI:10.1258/0969141053279130. PMID 15814020. Research Blogging.
- ↑ Hrung J, Sonnad S, Schwartz J, Langlotz C (1999). "Accuracy of MR imaging in the work-up of suspicious breast lesions: a diagnostic meta-analysis.". Acad Radiol 6 (7): 387-97. PMID 10410164.
- ↑ Morrow M (2004). "Magnetic resonance imaging in breast cancer: one step forward, two steps back?". JAMA 292 (22): 2779-80. PMID 15585740.
- ↑ Thomas DB, Gao DL, Ray RM, et al (2002). "Randomized trial of breast self-examination in Shanghai: final results". J. Natl. Cancer Inst. 94 (19): 1445-57. PMID 12359854. [e]
- ↑ Harris R, Kinsinger LS (2002). "Routinely teaching breast self-examination is dead. What does this mean?". J. Natl. Cancer Inst. 94 (19): 1420-1. PMID 12359843. [e]
- ↑ Rusiecki JA, Holford TR, Zahm SH, Zheng T. Breast cancer risk factors according to joint estrogen receptor and progesterone receptor status. Cancer Detect Prev 2005;29:419-26
- ↑ accessed 1/30/07 cancer.gov
- ↑ "FDA Approves New Breast Cancer Test". Associated Press, February 6, 2007.
- ↑ 80.0 80.1 (2006) "Sentinel Lymph Node Biopsy for Breast Cancer and Melanoma". Oncology Issues March/April: 22–5.
- ↑ cancer.gov
- ↑ Vaidya J. TARGIT (TARGeted Intraoperative radioTherapy). Retrieved on 2007-03-11.
- ↑ Vaidya J, Tobias J, Baum M, Houghton J. Protocol 99PRT/47 Targeted Intraoperative radiotherapy (Targit) for breast cancer. Retrieved on 2007-03-11.
- ↑ Vaidya J, Baum M, Tobias J, Massarut S, Wenz F, Murphy O, Hilaris B, Houghton J, Saunders C, Corica T, Roncadin M, Kraus-Tiefenbacher U, Melchaert F, Keshtgar M, Sainsbury R, Douek M, Harrison E, Thompson A, Joseph D (2006). "Targeted intraoperative radiotherapy (TARGIT) yields very low recurrence rates when given as a boost". Int J Radiat Oncol Biol Phys 66 (5): 1335-8. PMID 17084562.
- ↑ Targit literature Website
- ↑ Breast tumour drug target found, BBC News, 20 May 2007
- ↑ Wang, L et al (2005). "The inhibitory effect of flaxseed oil on the growth and metastasis of estrogen receptor negative human breast cancer xenografts is attributed to both its lignan and oil components". International Journal of Cancer 116 (5): 793-8. PMID 15849746.
- ↑ Thompson, LU et al (2005). "Dietary flaxseed alters tumor biological markers in postmenopausal breast cancer". Clinical Cancer Research 11 (10): 3828-35. PMID 15897583.
- ↑ Chen, J et al (2004). "Dietary flaxseed enhances the inhibitory effect of tamoxifen on the growth of estrogen-dependent human breast cancer (mcf-7) in nude mice". Clinical Cancer Research 10 (22): 7703-11. PMID 15570004.
- ↑ Chen, J et al (2002). "Dietary flaxseed inhibits human breast cancer growth and metastasis and downregulates expression of insulin-like growth factor and epidermal growth factor receptor". Nutrition and Cancer 43 (2): 187-92. PMID 12588699.
- ↑ Ali Fawzi, MD (June 2006). Gynecomastia. eMedicine.com. Retrieved on 2007-04-17.
- ↑ Armando E. Giuliano, MD (May 31 2006). Carcinoma of the Male Breast - General Considerations. Breast Cancer. Armenian Health Network, Health.am. Retrieved on 2007-02-27.
External links
General
- American Cancer Society - Learn About Breast Cancer Page
- History of breast cancer treatment
- The Breast: Neoplasms of the Breast
- Breast Cancer Care (UK charity)
- Abortion and Breast Cancer
- National Cancer Institute: Breast Cancer
- Breast Cancer Campaign (UK research charity)
Research and statistics
- International Agency for Research on Cancer home page
- Breast cancer incidence by country
- NSABP- Breast Cancer Research Clinical Trials Group
Clinical
- RadiologyInfo - The radiology information resource for patients: Breast Cancer
- Surgery Choices for Women with Early-Stage Breast Cancer, National Cancer Institute
- Mastectomy vs.n Lumpectomy: Who Decides?, National Research Center for Women & Families
- Australia: Cancer Control Bulletin Alcohol and cancer risk
- Cornell University Alcohol and the Risk of Breast Cancer
Other
- Pages with reference errors
- Pages using PMID magic links
- CZ Live
- Health Sciences Workgroup
- Biology Workgroup
- Oncology Subgroup
- Obstetrics and gynecology Subgroup
- Articles written in British English
- All Content
- Health Sciences Content
- Biology Content
- Oncology tag
- Obstetrics and gynecology tag
- Pages with broken file links