Staphylococcus aureus: Difference between revisions
imported>Andrew QC Lee No edit summary |
imported>Andrew QC Lee |
||
| Line 81: | Line 81: | ||
Studies are conflicting whether screening patients upon admittance to the hospital reduces nosocomial MRSA infections. A study of surgical patients was negative<ref name="pmid18334690">{{cite journal |author=Harbarth S, Fankhauser C, Schrenzel J, ''et al'' |title=Universal screening for methicillin-resistant Staphylococcus aureus at hospital admission and nosocomial infection in surgical patients |journal=JAMA |volume=299 |issue=10 |pages=1149-57 |year=2008 |pmid=18334690 |doi=10.1001/jama.299.10.1149 |url=http://jama.ama-assn.org/cgi/pmidlookup?view=long&pmid=18334690 |issn=}}</ref>, while a study was that screened all admissions was positive.<ref name="pmid18347349">{{cite journal |author=Robicsek A, Beaumont JL, Paule SM, ''et al'' |title=Universal Surveillance for methicillin-resistant Staphylococcus aureus in 3 affiliated hospitals |journal=Ann. Intern. Med. |volume=148 |issue=6 |pages=409-18 |year=2008 |pmid=18347349 |doi= |issn=}}</ref> In the positive study the patients received "5-day regimen comprising mupirocin calcium, 2% twice daily to the nares, and a chlorhexidine 4% wash or shower every 2 days" while in the negative study, patients who were found to have MRSA received "nasal mupirocin ointment and chlorhexidine body washing" without further details provided. | Studies are conflicting whether screening patients upon admittance to the hospital reduces nosocomial MRSA infections. A study of surgical patients was negative<ref name="pmid18334690">{{cite journal |author=Harbarth S, Fankhauser C, Schrenzel J, ''et al'' |title=Universal screening for methicillin-resistant Staphylococcus aureus at hospital admission and nosocomial infection in surgical patients |journal=JAMA |volume=299 |issue=10 |pages=1149-57 |year=2008 |pmid=18334690 |doi=10.1001/jama.299.10.1149 |url=http://jama.ama-assn.org/cgi/pmidlookup?view=long&pmid=18334690 |issn=}}</ref>, while a study was that screened all admissions was positive.<ref name="pmid18347349">{{cite journal |author=Robicsek A, Beaumont JL, Paule SM, ''et al'' |title=Universal Surveillance for methicillin-resistant Staphylococcus aureus in 3 affiliated hospitals |journal=Ann. Intern. Med. |volume=148 |issue=6 |pages=409-18 |year=2008 |pmid=18347349 |doi= |issn=}}</ref> In the positive study the patients received "5-day regimen comprising mupirocin calcium, 2% twice daily to the nares, and a chlorhexidine 4% wash or shower every 2 days" while in the negative study, patients who were found to have MRSA received "nasal mupirocin ointment and chlorhexidine body washing" without further details provided. | ||
==References== | ==References== | ||
Revision as of 13:50, 8 April 2008
Articles that lack this notice, including many Eduzendium ones, welcome your collaboration! |
| "Staphylococcus aureus" | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
 | ||||||||||||
| Scientific classification | ||||||||||||
| ||||||||||||
| Species | ||||||||||||
|
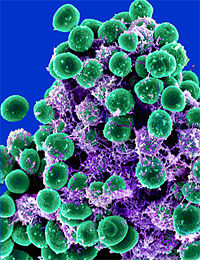
Staphylococcus aureus |
Description and significance
Staphylococcus aureus is a gram-positive spherical cocci that grows in a loose, irregular cluster resembling clusters of grapes. The cluster formation is due to the cell division occuring in three planes, with the daughter cell remaining in close proximity.[1] Staphylococcus aureus may also be found singly, in pairs and in short chains of three or four cells. The bacterium can never be found in long chains. They are non-motile and non-sporing. On an ordinary medium, Staphylococcus aureus can grow within a temperature range of 10-42°C. The optimum pH ranges in between pH 7.4-7.6. The bacteria thrives best in an oxygen rich environment. S. aureus can grow on all common laboratory media such as milk, nutrient gelatin or agar. When grown on a nutrient agar and incubated for 24 hours the colonies appear to be 2-4mm in diameter. The colonies appear circular, smooth, convex, shiny, and opaque.
Staphylococcus aureus was first observed in 1871 by von Recklinghausen. In 1880 Pasture obtained cultures of the bacteria and inoculated them into rabbits. Then in 1881 a surgeon by the name of Alexander Ogston documented two kinds of micrococci. The already known streptococci, arranged in chains and the other cocci arranged in clusters. Ogston named the cocci cluster Staphylococci because “Staphyle” in Greek means "bunches of grapes" and “kokakos” meaning a "berry". Unfortunately, Ogston did not provide a description of the genus and therefore it was not recognized. In 1884 Rosenbach successfully isolated and grew Staphylococcus aureus from pus. Rosenbach is credited with proposing the genus Staphylococcus and the species Staphylococcus aureus. He kept the genus name Staphlococcus because the bacteria was similar to that studied by Ogston. Rosenbach proposed the nomenclature for Staphylococcus aureus based on the yellow pigmentation of the colony.
In recent years the Staphylococcus aureus species has become a serious health issue. The bacteria has built up a strong resistance to treatment. By unlocking the genome sequence, researchers could understand the nature of its resistance, virulence, genetic flexibility, epidiology and physiology. Comparing the genome sequence of S. aureus with the genomes of a less virulent form and nonpathogenic species could help researchers have a better understanding of the nature of Staphylococcal aureus infections.[2]
Describe the appearance, habitat, etc. of the organism, and why it is important enough to have its genome sequenced. Describe how and where it was isolated. Include a picture or two (with sources) if you can find them.
Genome structure
The Staphylococcus aureus genome contains about 2.800 to 2.903 million base pairs of DNA. The bacteria has about 2,600 genes in its chromosome. The first whole genome sequence of S. aureus strains were completed by shot-gun random sequencing in 2001. S. aureus plasmids contains genes that encode resistance to antibiotics, heavy metals, or antiseptics. Some virulence genes have been reported to be carried on plasmid, such as exfoliative toxin B and some superantigens.[6] Approximatly 75% of S. aureus genome comprises a core component of genes present in all of the strains.[7]
Describe the size and content of the genome. How many chromosomes? Circular or linear? Other interesting features? What is known about its sequence?
Does it have any plasmids? Are they important to the organism's lifestyle?
Cell structure and metabolism
Staphylococcus aureus can be found in spherical clusters with a thick peptidoglycan layer of cell wall. Some young cultures posses microscopically visible capsules. Many noncapsulated strains of S.aureus have small amounts of capsular material on the surface.
Staphylococci are facultative anaerobes that grow by aerobic respiration or by fermentation that yields lactic acid. S. aureus ferments sugars by producing acid but no gas.
Phagocytosis is a mechanism used by the host organism to combat a staphylococcal infections. S. aureus produces leukocidin, which cause the distruction of leukocytes allowing the bacteria to escape phagocytosis. Leukocidin is produced in skin lesions such as boils which results in cell distruction of white blood cells and is one of the factors responsible for pus formation.
Describe any interesting features and/or cell structures; how it gains energy; what important molecules it produces.
Ecology
Staphylococcus aureus is commonly found on the skin and in various mucous membranes of man and other animals. About 20-30% of healthy people in the United States are carriers of the bacteria.[3] These individuals are usually unaware that they are carriers of the bacteria and usually never get sick from it. In hospitals the percentage is higher because of more possible contact with infected cases.
Describe any interactions with other organisms (included eukaryotes), contributions to the environment, effect on environment, etc.
Pathology
Staphylococcus aureus is one of the most common pathogenic bacteria. The organism may cause disease through tissue invasion and toxin production. The bacteria could cause a wide range of infections both internally and externally. It may cause skin infections, bone infections, pneumonia, food poisoning, Toxic shock syndrome, life threatening bloodstream infections and other serious illnesses.
Staphyolococcus aureus may cause boils usually by entering the skin through a hair folicle or a cut. They may be red, swollen and painful, and sometimes have pus. They can turn into impetigo, which turns into a crust on the skin. The organism could also cause internal abscesses. In recent years Staphylococcus aureus has become one of the leading causes of hospital acquired infections. People prone to staphylococcal infections include newborns, drug users; breastfeeding women; and people with skin disorders, surgical incisions, a weakened immune system, or chronic diseases[4]
Staphylococcus aureus has a high incidence of drug resistance with methicillin-resistant strains resistant to ß-lactams and most other antibiotics. Infections are enhanced in the presence of foreign materials inside the body such as tampons, surgical packing or intravenous catheters.[5]
Treatment is usually unnecessary but can be treated with an antibiotic. Maintaninting good hygiene and avoiding contact with exposed outbreaks could prevent spreading the bacteria.
How does this organism cause disease? Human, animal, plant hosts? Virulence factors, as well as patient symptoms.
Application to Biotechnology
In an anaerobic environment Staphylococcus aureus can reduce mannitol to lactic acid, which differentiates it from other species of staphylococci. The bacterium is the only coagulase positive and ß-hemolytic staphylococcus. When grown on a nutrient agar containing phenolphtalein diphosphate the bacterium produces phosphatase. When ammonia vapor is introduced to the culture, the colonies assume a bright pink color due to the presence of free phenophalein. Researchers use this test to distinguish between Staphylococcus aureus from S. epidermidis.
Does this organism produce any useful compounds or enzymes? What are they and how are they used?
Current Research
Enter summaries of the most recent research here--at least three required
Methicillin-resistant staphylococcus aureus
Methicillin-resistant staphylococcus aureus (MRSA) is a variety of staphylococcus that is resistant to commonly used antibiotics such as methicillin. MRSA has become an important public health problem.[1][2]
Screening for MRSA
Studies are conflicting whether screening patients upon admittance to the hospital reduces nosocomial MRSA infections. A study of surgical patients was negative[3], while a study was that screened all admissions was positive.[4] In the positive study the patients received "5-day regimen comprising mupirocin calcium, 2% twice daily to the nares, and a chlorhexidine 4% wash or shower every 2 days" while in the negative study, patients who were found to have MRSA received "nasal mupirocin ointment and chlorhexidine body washing" without further details provided.
References
- ↑ Klevens RM, Morrison MA, Nadle J, et al (2007). "Invasive methicillin-resistant Staphylococcus aureus infections in the United States". JAMA 298 (15): 1763–71. DOI:10.1001/jama.298.15.1763. PMID 17940231. Research Blogging.
- ↑ Sack K (2007). Deadly Bacteria Found to Be More Common. Retrieved on 2008-01-03.
- ↑ Harbarth S, Fankhauser C, Schrenzel J, et al (2008). "Universal screening for methicillin-resistant Staphylococcus aureus at hospital admission and nosocomial infection in surgical patients". JAMA 299 (10): 1149-57. DOI:10.1001/jama.299.10.1149. PMID 18334690. Research Blogging.
- ↑ Robicsek A, Beaumont JL, Paule SM, et al (2008). "Universal Surveillance for methicillin-resistant Staphylococcus aureus in 3 affiliated hospitals". Ann. Intern. Med. 148 (6): 409-18. PMID 18347349. [e]
http://www.nih.org/NIHnewWebsite/nihPublicHealth/pdfs/MRSAParentsGuide.pdf